Written by Emily Klosterman, DVM, MS, DACVIM
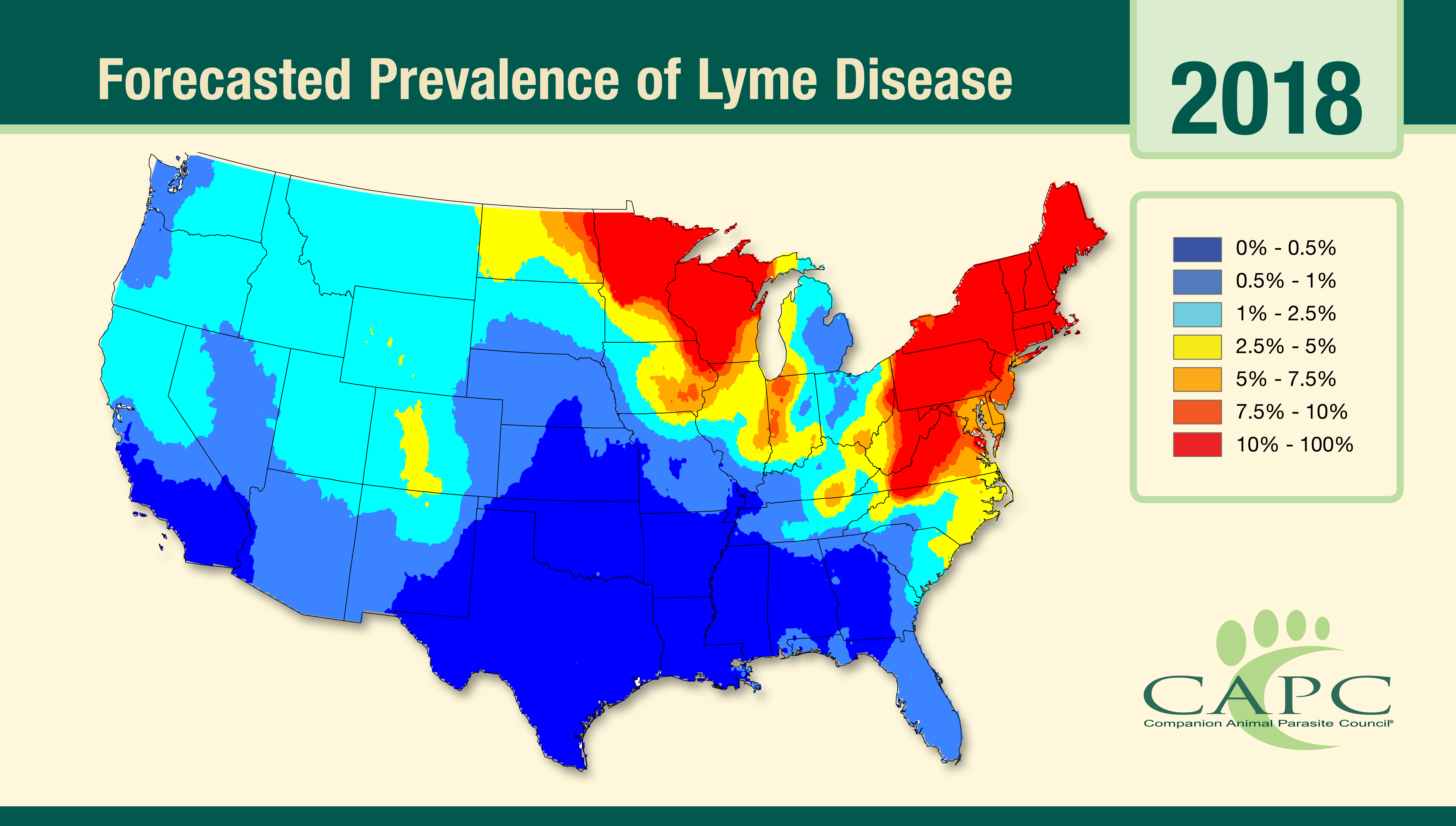
Pennsylvania and other states along the eastern seaboard are common places where dogs might contract Lyme disease. Recognizing the signs of Lyme disease can lead to quicker diagnosis and treatment. However, the disease can manifest in many different ways, thus making it difficult for even the most vigilant of dog owners to know that their pet has Lyme disease.
Lyme disease is a bacterial infection transmitted by tick bites. The bacteria (Borrelia burgorferi) lives in the digestive system of the tick and infects the dog through the tick’s saliva. The bacteria can move around the body and evades detection by the immune system much better than other bacterial infections which makes it a disease that can cause many types of clinical signs. Because the bacteria are so good at hiding in the body, even with antibiotic treatment many dogs are never cured of this infection.
Incidentally discovered infection
Many dogs are found to be Lyme disease positive when tested, but fortunately few have signs of disease and the positive test is found with routine screening. A Lyme disease test is incorporated into many general health labwork panels and is also included in many in-clinic tests for heartworm disease. In areas where Lyme disease is common, screening can identify dogs that might need more attention. Screening can also identify dogs that have had previous exposure to the infection but no longer have an active infection (which doesn’t require treatment).
When a dog tests positive, further testing to measure the significance of the body’s immune response is recommended with a test called the quantitative C6 antibody titer test. This test allows your veterinarian to better understand whether your pet has a newer or older infection. Dogs with a low titer probably had their infection in the past or their immune system fought off the infection and do not require treatment. If your pet has a high C6 antibody titer but no clinical signs then their body may be taking care of the infection on its own and treatment with antibiotic may be unnecessary. Sometimes, a veterinarian may recommend antibiotic treatment for dogs with no clinical signs and significant C6 antibody titers. Antibiotics might be recommended in pets with reduced immune system function or in an attempt to prevent some of the more serious manifestations of Lyme disease discussed below. Finally, if your pet has tested positive for Lyme disease your vet will likely recommend testing for excessive protein in the urine. Protein in the urine is a manifestation of Lyme disease that can damage the kidneys but can go unnoticed unless tested for regularly.
Lyme arthritis
One form of active Lyme disease is characterized by fever, swollen lymph nodes, muscle soreness and arthritis. Once the bacteria are transmitted to the dog, they move around the body triggering swelling and inflammation as they travel. The joints appear to be very sensitive to this inflammation and chronic arthritis can become a problem in these pets. In addition, as discussed previously, sometimes the bacterial infection is never completely cleared from the body and chronic infection in the joint is possible. Cases of disease with chronic joint inflammation are complex and so your family veterinarian may recommend that your dog visit a veterinary specialist.
Lyme nephritis
The most devastating way a pet can be affected by Lyme disease is severe kidney inflammation (Lyme nephritis). Dogs are often diagnosed with this type of Lyme disease when they have signs like poor appetite, vomiting or lethargy and then blood tests performed at the veterinarian’s office reveal kidney failure. Immediate antibiotic treatment is recommended in these patients, but unfortunately the inflammation in the kidney triggered by the bacteria is often so severe that the kidneys continue to fail and never recover. Sadly, many dogs affected by Lyme nephritis will suffer the effects of kidney failure for the rest of their life and ultimately may die from severe kidney failure in a few weeks or months. Outcome in these dogs mostly depends on the severity of the kidney failure, but evaluation by a veterinary internal medicine specialist may help maximize quality of life for as long as possible.
Secondary autoimmune disease
Lyme disease can affect many different organs in the body and this can lead to autoimmune diseases (where the body inappropriately attacks its own tissues). Autoimmune disease is not directly caused by the bacteria and so even after antibiotic treatment pets can remain sick. Autoimmune blood or joint disorders are most commonly seen and require a specialized treatment course completely separate from the antibiotics for Lyme disease.
Prevention
The longer a tick is attached to its host (esp. > 48 hours) the more likely it is that Lyme disease will be contracted so limiting the time a tick spends on your dog’s body is an important preventative measure. Looking for ticks on your pet’s body can be helpful, but ticks that are not yet fully grown can transmit Lyme disease and they can be too small for you to see or feel. Use of tick preventative medication is an important way to limit the time a tick might spend on your dog’s body.
The Lyme disease vaccination is a unique vaccine in that it is not meant to fight the infection once it is in the body, but is designed to prevent transmission from the tick. The vaccine attempts to fill a vaccinated dog’s blood with antibodies that will kill the bacteria in the tick’s stomach before it even enters your dog’s body. Lyme disease vaccination is recommended in dogs that live in or travel to high risk areas.
Keep a close eye on your dogs during tick season this year and cat lovers take heart, cats are generally considered resistant to Lyme disease. People cannot get Lyme disease from their dog; however, you can contract the disease from a tick too. Be aware that if your dog is being bitten by ticks carrying Lyme disease then your family could be bitten too.